MM Curator summary
After years of effort and multiple political challenges, North Carolina HHS officials have brought managed care to the state for the first time.
The article below has been highlighted and summarized by our research team. It is provided here for member convenience as part of our Curator service.
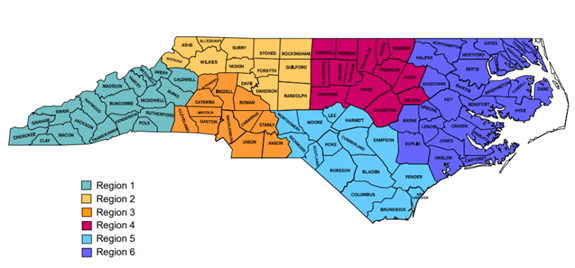
A map shows North Carolina’s managed care regions. The state is switching to a new Medicaid system Thursday.
Thursday is a big day for Medicaid in North Carolina.
The state is officially switching to a new Medicaid system called a “managed care” model.
That means 1.6 million Medicaid recipients will receive health care through plans managed by a small group of companies. Instead of paying doctors directly for their services, the state will pay companies that will then pay doctors who treat Medicaid recipients.
About 40 other states use this model, according to the Kaiser Family Foundation. The goal is to save money and improve care.
But it will likely be a bumpy transition. Very few people in North Carolina have chosen their own health plan, according to state data, and many likely don’t even know the change is happening.
An advocacy group called North Carolina for Better Medicaid surveyed 170 Medicaid beneficiaries and found that 43% of them knew “very little” or “nothing” about the switch to managed care. Dave Richard, the head of NC Medicaid, said that’s not surprising.
“We tried to do everything we could — reach out with social media, with radio and television media, direct mail-outs to beneficiaries,” Richard said. “But people’s lives are complicated and a lot of things are going on.”
Becca Friedman with the Charlotte Center for Legal Advocacy said she is particularly worried about problems with the mail.
“There’s definitely been a lot of notices that have gone out to beneficiaries that we’re nervous aren’t getting to them,” Friedman said.
She said a lot of Medicaid beneficiaries have moved or changed their addresses during the pandemic and the state may not have their updated mailing information.
Medicaid recipients had until May 21 to pick their own new health plan or the state would automatically assign one. According to Richard, only about 15% of people signed up, which he said is in line with what other states saw when they changed systems.
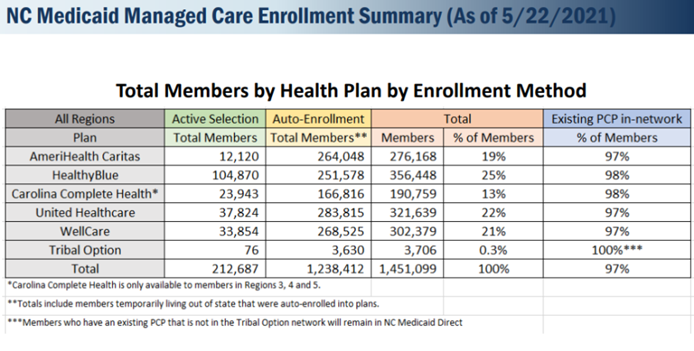
NCDHHS
“We would love to have had it higher,” Richard said. “But in consultation with other states who had gone live with managed care … it’s well within the norms that they experienced.”
Richard said the state based its health plan assignments for the other 85% of Medicaid recipients around people’s primary care doctors so that people could theoretically continue to see the same provider. He admits there will be problems with the auto-assignments.
For example, he said, the primary care doctor that the state has on file for someone might be outdated and not match the doctor that they have actually been seeing. Or their new plan might not include a specialist that they need.
“If you have heart disease … your primary care provider is really, really important. But your cardiologist is probably more important to you,” Richard said. “You may not have been assigned to a plan where your cardiologist is enrolled.”
Richard said he and his staff are bracing for a flood of phone calls and emails in the coming weeks and the state has planned for some hiccups. If a Medicaid recipient shows up for an appointment and the doctor isn’t on their new plan, that doctor can still bill Medicaid for the next 60 days.
“We have a rapid response team that’s ready, prepared to do this,” Richard said. “Our health plans are all ready for that. Our enrollment broker will continue to be there to address beneficiary issues.”
Recipients have until Sept. 30 to change their managed care plan for any reason.
Want to read all of WFAE’s best news each day? Sign up here for The Frequency, WFAE’s daily email newsletter, to have our top stories delivered straight to your inbox.
Clipped from: https://www.wfae.org/health/2021-06-30/big-change-to-nc-medicaid-system-takes-effect-thursday
